Protecting Health, Sharing Information

At the beginning of 2020, hardly anyone had heard of COVID-19. As this devastating disease quickly swept across the globe, clinicians scrambled to learn how best to treat it and prevent its spread.
In the UCSF Division of Cardiology, Nisha Parikh, MD, MPH, has led the development of clinical guidelines to provide the very best care, and to keep patients, doctors and staff as safe as possible. “We really came together as a group to develop protocols for how to interact with patients safely in the clinic, echocardiography lab, cardiac catheterization lab, and cardiac intensive care unit (ICU),” she said. “Of course, much of this is a moving target, and we’ve learned a lot about the disease.” She and her colleagues have posted these evolving guidelines online (bit.ly/covidcardio) as a resource for other institutions as they develop their own guidelines.
In cardiology, one of the highest-risk procedures for COVID-19 transmission is a transesophageal echocardiogram (TEE), in which a cardiologist inserts a probe into a patient’s mouth and down the esophagus in order to provide a detailed look at the heart. “TEEs can be aerosol-producing procedures,” said Dr. Parikh. “So even if a patient tested negative for COVID, we assume that they could have it, and have our team wear N95 masks and full face shields.”
Dr. Parikh also worked with Jamie Kennedy, MD, medical director of the cardiac ICU, Benjamin Kelemen, MD, a cardiology fellow, and others to develop a list of recommended lab tests that could help assess cardiac dysfunction. These include including cardiovascular biomarkers like troponin, which can indicate possible heart damage and could indicate a worse prognosis. For patients with mild to moderate COVID-19, the evidence suggests that there is no clinical benefit to taking patients off angiotensin-converting enzyme (ACE) inhibitors or angiotensin receptor blockers (ARBs).
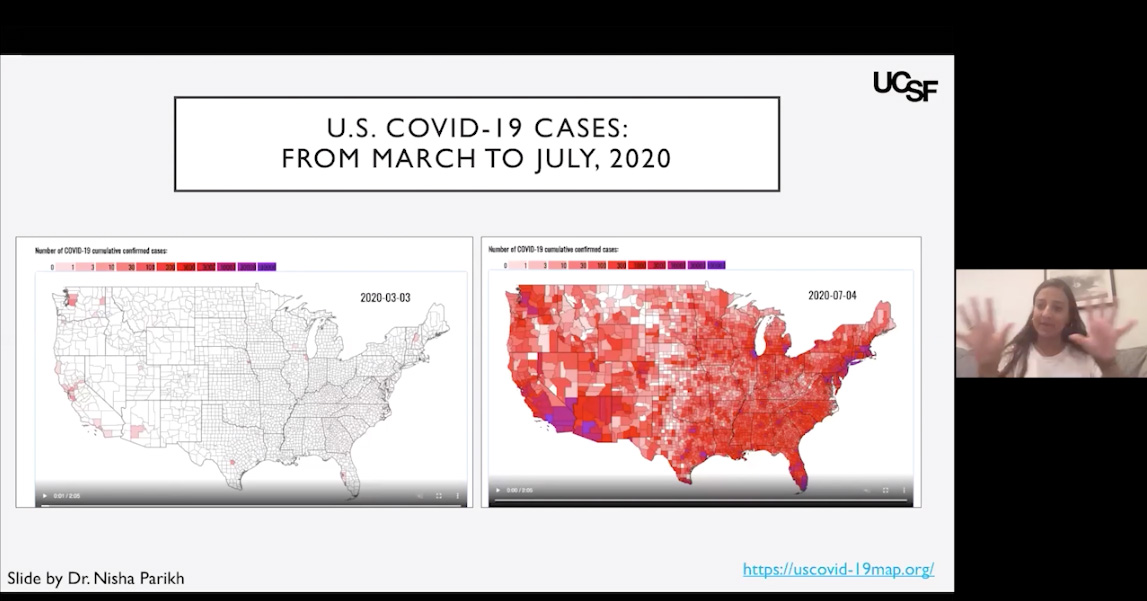
Because COVID-19 can have a particularly harmful effect on the lungs, cardiologists have learned that the disease can contribute to right ventricular dysfunction – since this chamber of the heart is the one that pumps blood to the lungs. They also monitor for hypercoagulability, or excessive blood clotting, since COVID- 19 can also contribute to this disorder. “A lot of what we put together was based on conversations with frontline colleagues from ‘hotspots’ around the country,” said Dr. Parikh. “Keeping those lines of communication open is very important, and will get us all through this.”
Don’t Delay Care
Perhaps the most important message for patients is to seek prompt treatment for urgent symptoms. “At the beginning of the pandemic, there was some confusing messaging about when to come in, but now the air has cleared,” said Dr. Parikh. “We’ve been doing this for a while, and we have a good sense of how to be safe in clinic. Please don’t ignore chest pain or shortness of breath. We definitely want patients to be seen for their heart symptoms, so we can prevent any long-term problems from developing.”
In addition to developing clinical guidelines, Dr. Parikh has coordinated a series of grand rounds and educational sessions for the community, including One Medical Group, community cardiovascular disease referral partners, and statewide associations of nurse practitioners and physician assistants. Her co-presenters included UCSF cardiologists Bruce Conklin, MD, and Krishan Soni, MD, MBA; UCSF cardiology fellows Joseph Bayne, MD, Dr. Kelemen, and Gregory Judson, MD; and guest presenter Daniel Sims, MD, medical director of the Montefiore Medical Center cardiac ICU in the Bronx.
“At UCSF, we are very lucky to have access to all sorts of town halls and grand rounds presented by world leaders,” said Dr. Parikh. “We in turn distilled all that great information and provide it to our community partners. These forums are attended by hundreds of people, and everyone is so appreciative. It’s really heartwarming to see the ways that this pandemic is bringing everyone together. There’s been so much great teamwork, from putting together these educational activities to developing clinical guidelines. We’re all learning from each other."
